Send Vaccines Where People Want Them: Developing Nations
According to a new study co-authored by Yale’s Mushfiq Mobarak and Saad Omer, COVID-19 vaccine acceptance is significantly higher in low- and middle-income countries than wealthy ones. The results suggest that prioritizing developing nations for vaccine distribution could help save more lives and keep variants at bay.
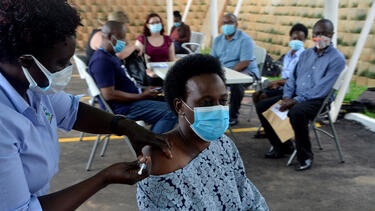
A COVID-19 vaccination site in Uganda, one of the countries surveyed in the study, in May 2021. Photo: Nicholas Kajoba/Xinhua via Getty Images.
In the United States, where COVID-19 vaccines are plentiful, the biggest remaining obstacle to protecting the population is vaccine hesitancy. Meanwhile, public health experts are raising the alarm that the highly contagious Delta variant is spreading through unvaccinated populations—and additional variants could arise as long as the disease is endemic. But according to a new study, once more vaccines are made available in the developing world, there will be plenty of people eager to receive them—a finding that underscores the importance of global vaccine equity in saving lives and preventing the evolution of new, more dangerous variants.
Willingness to get the COVID-19 vaccine is significantly higher in low- and middle-income countries (LMICs) than in the United States or Russia, according to the study on global COVID-19 vaccine acceptance and hesitancy, whose co-authors include Mushfiq Mobarak of Yale SOM and Saad Omer, director of the Yale Institute for Global Health.
The research drew on phone surveys of more than 44,000 people in the United States, Russia, and 10 low- and middle-income countries (LMICs) across Asia, Africa, and South America, administered between June 2020 and January 2021. Respondents were asked about their willingness to take the COVID-19 vaccine when available, as well as their motivations for taking it, concerns about it, and most trusted source of vaccine information. The authors include scholars from Innovations for Poverty Actions, the International Growth Center, the Yale Research Initiative on Innovation and Scale, WZB Berlin Social Science Center, and other institutions in countries around the world.
The goal of the research, Mobarak explains, was to establish a clearer understanding of global vaccination attitudes by using a large and diverse sample of countries. “Before designing any interventions to overcome vaccine hesitancy, we’re trying to understand the basic facts,” he says.
With this foundational information in hand, the researchers hope to shift “from hunch-based policy to evidence-based policy,” Omer says.
The survey responses revealed notably different attitudes toward the COVID-19 vaccine between wealthy and less wealthy nations, with 80.3% of people in LMICs expressing willingness to get the vaccine when available. Just 64.6% percent of Americans and 30.4% of Russians said the same.
“If the goal is to maximize global vaccination coverage, distributing vaccines to countries in Asia and Africa that don’t currently have them is going to be a lot easier and cheaper than trying to convince the last 30 percent of Americans.”
To Mobarak, the high levels of acceptance in LMICs suggest that prioritizing distribution to these countries could have important benefits. “If the goal is to maximize global vaccination coverage, distributing vaccines to countries in Asia and Africa that don’t currently have them is going to be a lot easier and cheaper than trying to convince the last 30% of Americans to get vaccinated,” he says.
Improving access in LMICs, where vaccination rates are currently extremely low, could also help to prevent the emergence and spread of new COVID-19 variants. “If we ended up with a new variant coming out of Latin America, Africa, or Asia, and the Pfizer and Moderna vaccines are not effective against it, then we’re basically back to square one,” Mobarak explains. “Our paper shows that distributing vaccines to the rest of the world would be a high-return activity, because most people there are ready to take it.”
Why are wealthier nations so much more hesitant than LMICs? While the survey results don’t directly address this question, the researchers have a few theories. “In a lot of low- and middle-income countries, the pandemic response—good or bad—has been a national response,” says Omer. “Unfortunately, in a lot of high-income countries, it’s been a political response. So that’s part of it. If you politicize a response, you lose half the country one way or another.”
Residents of LMICs also have more recent experiences with the life-saving benefits of other vaccines. “People have the memory—both personal and institutional—of diseases like measles and polio,” Mobarak notes. “People know what problems non-vaccination can cause.”
Hearteningly, the survey results also suggest that most vaccine hesitancy does not appear to be especially deep-rooted. Among vaccine-hesitant survey respondents, the most commonly cited reason for reluctance was concern about side effects; relatively few, except in Russia and Burkina Faso, mentioned conspiracy theories.
“The concerns are really of a health expertise nature,” Mobarak says. “Like, ‘I’m worried about side effects,’ or ‘I’m worried about whether this vaccine is really effective.’ Which are rational concerns, and not irrational things, like ‘Somebody is using this vaccine to implant a chip in me.’”
“It’s not that conspiracy theories are not important, and it doesn’t mean that they won’t play a role going forward,” Omer adds. “But at this point, it’s the basic characteristics of the vaccines that people are talking about.”
In high- and low-income countries alike, respondents reported that health workers were their most trusted source of vaccine information, followed by the government in some countries and friends and family in others. Celebrities received low marks, suggesting the limits of star-studded vaccine rollout efforts.
“Even amongst those who are skeptical of vaccines, the most trusted source of vaccine information remains healthcare providers,” Omer says. “That’s important to keep in mind as we deploy a strategy. So yes, a soccer player can attract attention to the vaccine issue, but they do not replace healthcare workers as a trustworthy source.”
For high-income nations, the challenge ahead is to use this knowledge to overcome lingering hesitancy. Omer is particularly concerned about Russia’s strikingly low rates of acceptance. “That really doesn’t bode well for us, because you cannot effectively control or eliminate the disease in large regions if you have that high level of skepticism around vaccines,” he says.
In LMICs, governments and policy makers will have to translate people’s willingness to get the vaccine into action. “There are ways of making the process of actually getting the jab easier for people,” Mobarak says. Vaccination vans could travel through cities and towns. In rural communities, governments could use local schools and clinics to distribute vaccines to anyone who arrives on pre-announced days.
Ultimately, the research suggests that establishing global vaccine equity is the most efficient way out of the pandemic. Getting vaccines to LMICs where rates are low is “even in the selfish interest of other rich countries, because you really don’t want new variants to emerge,” Mobarak says.
The rates of vaccine acceptance in LMICs look high compared to the U.S. and Russia but even those aren’t high enough to reach herd immunity, so governments in the developing world will have to increase supply of and demand for the vaccine at the same time. “There’s hope in low- and middle-income countries, but we have our work cut out for us,” Omer says. “The glass is truly half-full and half-empty.”