Uncovering the Mental Health Impacts of COVID-19 in Low- and Middle-Income Countries
A new study co-authored by Yale SOM’s Mushfiq Mobarak investigated how mental health fared after the pandemic arrived in eight low- and middle-income countries, and found signs of a sharp, and lasting, deterioration. Now he is training his sights on possible solutions.
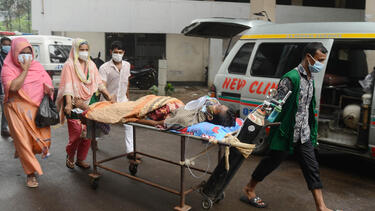
A COVID-19 patient is taken to a hospital in Dhaka, Bangladesh, in July 2021.
The COVID-19 pandemic has wreaked havoc on mental health, and its consequences linger. One large research review found that the pandemic increased the prevalence of depression by almost 28%. But so far, research have focused on richer countries, while the adverse mental-health response to COVID-19 outbreaks and lockdowns in low- and middle-income countries have garnered far less attention in academic research and policy discussions.
There’s reason to suspect that the blow delivered by the pandemic to individuals’ mental health could be worse in poorer countries, says Yale SOM’s Ahmed Mushfiq Mobarak. Mobarak’s own research has shown that the pandemic hit the economies of low- and middle-income countries hardest, often leading to widespread food shortages. These countries also have worse access to healthcare and less insurance coverage—and many of them received fewer COVID-19 vaccines.
“Mental health problems are big, and during the pandemic, they got bigger. And we really don’t have the infrastructure or the resources to deal with this. It will require some creative solutions.”
For a new study, published this month in PLOS Medicine, Mobarak collaborated with Nursena Aksünger, a PhD candidate at Vrije Universiteit Amsterdam; Corey Vernot, a research associate at Yale; and an international team of researchers to investigate how the pandemic affected the incidence of depression in eight low- and middle-income countries in South Asia, Sub-Saharan Africa, and South America. The research team conducted repeated surveys of over 20,000 people, spanning a period from before the pandemic to 15 months after its onset.
The researchers’ findings were sobering: not only did they reveal a “large, significant, negative impact of the pandemic on mental health,” but those impacts also appeared to persist beyond their severest point in the early months of lockdown. “We do not see a clear sign of mental health fully bouncing back to pre-pandemic levels,” they write.
Mobarak hopes the paper’s striking findings will act as a wake-up call to policymakers and others with the power to implement public mental health interventions.
“We are noticing that these [mental health] problems are big, and during the pandemic, they got bigger,” Mobarak says. “And we really don't have the infrastructure or the resources to deal with this. It will require some creative solutions.”
The new paper grew from a research project Mobarak began before the pandemic, and on a very different research question: whether the provision of loans could help to address seasonal food insecurity in Nepal.
When the pandemic hit, Mobarak’s research team continued regularly interviewing their subjects in Nepal over the phone. At the same time, they launched a series of survey-based projects in other countries that sought to quantify the scope of pandemic-related economic losses.
“We wanted to try to look at different ways in which this pandemic might have persistent effects on people’s lives that we’ll have to worry about in the future,” Mobarak says. “Mental health was one such area.”
Mobarak set out to find other researchers conducting the kind of survey-based data collection that could help broaden the foundation of his own project, expanding its scope and geographic reach. To fit into his study, other researchers’ data needed to have specific characteristics—for example, they had include a pre-pandemic survey period and repeated rounds of interviews of the same subjects.
In the end, the paper’s data consists of ten different sample groups, totaling 21,162 individuals, across Bangladesh, Colombia, Democratic Republic of the Congo, Kenya, Nepal, Nigeria, Rwanda, and Sierra Leone.
Taking multiple rounds of sample group surveys proved crucial, because they revealed predictable, within-year fluctuations in mental health driven by crop cycles. The researchers noticed that mental health tends to suffer in the pre-harvest “lean” period, and improve after a harvest. Methodologically, this was an important discovery because it signaled to the researchers that they needed to control for these seasonal variations to reveal the true impact of the pandemic on mental health.
“Those fluctuations can dwarf pandemic effects and risk conflating seasonality with the pandemic,” the authors write, “depending on the exact phase of the local crop cycle during which COVID-19 had arrived in a country.”
Even after controlling for cropping-related ups and downs, the researchers found that depression symptoms increased by around 0.3 standard deviations in the four months following the onset of the pandemic—a significant amount.
Especially concerning to the researchers is the fact that in the countries they studied, the infrastructure necessary to offer sorely needed mental health treatment is lacking. The World Health Organization reports that 82% of people living with a mental health disorder live in low- or middle-income countries, where annual mental health spending constitutes only $0.25 per person (compared with an average of just under $2 per person globally).
The solution, Aksünger says, is to develop models for affordable mental health treatment.
“To address the lack of mental health infrastructure in LMICs, policymakers should prioritize task-sharing and invest in frugal solutions such as training lay health workers and community-based care providers”—a concept similar to community health workers who offer immunization or neonatal health services. “By including this support in universal healthcare coverage, the accessibility and affordability of mental health services can be improved, making a significant difference in the lives of those who need it most.”
Mobarak’s research projects often aim to study the effectiveness of possible solutions to big problems, and that’s where he hopes to pivot next. The Yale Research Initiative on Innovation and Scale (Y-RISE), where Mobarak serves as faculty director, has teamed up with non-governmental development organization BRAC in Bangladesh to test the effectiveness of community-based lay mental health workers.
“We have to be thinking creatively about those types of solutions,” Mobarak says, “because the problem's there, and currently there's very little attention paid to it.”