Why Does Spending on Drugs Keep Going Up?
Eric Tichy ’18, vice chair of pharmacy formulary at the Mayo Clinic, is part of a team that reports each year on trends in drug expenditures. He explains what’s driving pharmaceutical spending and what it means for patients, providers, and pharma companies.
Q: This paper is part of a series published annually by the American Journal of Health-System Pharmacy. You’ve been the lead author for the last three years. What’s the goal of the series?
It helps healthcare organizations and policy makers understand trends with prescription drug expenditures. It gets a lot of attention because drug expenditures are always a hot topic. Even my parents are concerned about the cost of prescription drugs.
With COVID, the issue has become especially important because of all the new therapeutic agents that have become available. Thus far, the government has been paying for many of them, but we’re going to hit an inflection point where we return to traditional way of managing and paying for these pharmaceuticals which will impact the general public.
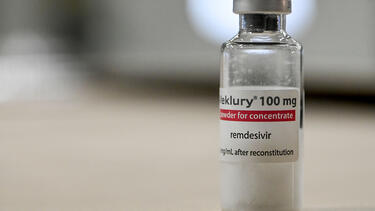
We’re already getting a hint of that. Remdesivir, the one COVID-related drug that was not paid for by the government, was the number one spend for hospitals. The $3.1 billion spent on it in hospitals was more than the next three drugs combined.
Q: Overall, in 2021 pharmaceutical expenditures in the U.S. were $576.9 billion. That’s up 7.7% from the prior year. However, those numbers don’t include the COVID vaccines or treatments that were paid for by the government. How are healthcare organizations preparing for the possibility that COVID will persist but the government coverage of therapeutics won’t?
It’s looking like COVID is not something that’s going to go away. In my role at the Mayo Clinic, I’m trying to project what kind of funds we need for COVID therapies in the future. Will we be doing annual COVID boosters in the fall, similar to what we do for flu vaccine? Will the government fund through this year? Through next year? Within healthcare organizations around the country there are real questions about, “If the government doesn’t fund, what are we going to do?”
My thought is it’s hard to move forward until the government makes a decision. Whatever the decision, I think we can figure out a way forward, but until then we can’t really plan or contract with manufacturers. At some point we need to move out of this public health emergency phase and transition to what we do with other disease management.
Q: What can patients learn from this paper?
From a patient perspective, I think there’s actually a lot of good things in the paper. There’s been trends overall in healthcare where more costs are being shifted to patients, and that amplifies concerns that patients have about increasing drug costs. But drug price inflation and consumer price inflation have diverged. At a time when inflation is around 8%, drug prices are relatively flat. We don’t know when the broader inflation is going to find its way into drug prices, but it’s a positive for the consumer right now.
“Generic drugs account for about 90 percent of the prescriptions filled each year, but only 20 percent of the spending. It’s the Pareto Principle: 10 percent of the drugs prescribed account for 80 percent of the cost.”
Generics have been an important factor moderating the cost of prescription drugs. Generic drugs account for about 90% of the prescriptions filled each year, but only 20% of the spending. It’s the Pareto Principle: 10% of the drugs prescribed account for 80% of the cost. But most of the really costly new medications developed over the last 20 to 30 years have been biological medications. There wasn’t a generic pathway for those, until recently—biosimilars are the equivalent of generic for biologic medications. Over the last three years biosimilars have really started to have a material impact. Their uptake is beginning to blunt the cost of drugs. That’s a positive development for consumers, and it’s going to continue to get better.
The number one drug expenditure overall was a drug called Humira. That will face biosimilar competition in 2023. Each year new generics and biosimilars become available and drive savings.
Within that realm, if I were guiding policymakers on ways to slow the growth of pharmaceutical expenditures, I would point them to the number of lawsuits that slow the introduction of generics and biosimilars.
Q: Do these positives for consumers mean challenges for pharmaceutical companies?
Pharmaceutical companies are certainly facing inflationary pressures, and it’s getting harder and harder to develop new therapies and to bring them to market successfully.
Last year a drug called Aduhelm for Alzheimer’s disease came out. Initially, it was exciting. It was one of the big hopes for pharma, but that turned to controversy as questions were raised about the cost and the quality of the data supporting its approval. In the end, essentially, the drug went nowhere.
That whole marketplace is potentially going to be slowed down as a result. For some time, the pharmaceutical industry’s return on investment numbers made it one of the more favorable sectors of the economy. Ten years ago, the development of new drugs by the pharmaceutical industry was probably easier and more lucrative than it is today.
Q: What drives the increase in expenditures on pharmaceuticals year after year?
When people see those top-line numbers on increases in drug expenditures, a lot of times they think it’s just that the prices went up. It’s important to understand that the increasing expenditures on pharmaceuticals come from three main factor: price increases, volume, and the mix of drugs. We’ve found that, over time, it’s pretty evenly distributed across those three factors. For the last five years, prices were not the main factor driving the increasing expenditures. Last year, healthcare organizations were very full and always busy, so there were huge increases in healthcare utilization—volume—coming from the COVID crisis and from trying to catch up on care deferred during the worst of the pandemic.
When the hepatitis C therapy came out and when immune checkpoint inhibitors were released as oncology therapies, those were both groundbreaking therapies, and they were very expensive. They changed the mix of drugs being used and increased spending a lot. However, the hepatitis C therapies have largely cured hepatitis C reducing long-term costs of care and have improved lives producing economic benefits.
Historically, we have also seen other difficult-to-predict events impact drug expenditures. For example, the H1N1 flu increased expenditures. Even things like hurricanes that cause enough devastation to produce drug shortages can show up in drug expenditure data. It’s hard to predict exactly what the thing is going to be, but there’s going to be something that causes a spike in one of the drivers, but there tends to be a return to the mean over time.
The good thing is when you have a lot of data you can cut it many different ways to understand the different trends that are going on. The series has nine co-authors. We’re a diverse group from different parts of the country and different practice areas. So, we each bring a different lens to the table. By looking at trends over time you see that even with something like COVID, things will normalize over time.