The History of the Forgotten Pandemic
In spring 1957, tens of thousands of refugees in Hong Kong fell ill with a novel strain of the flu. The virus would spread around the world, the first global outbreak since the 1918 flu pandemic and the first test of a fledgling early warning system. More than one million people died, 116,000 of them in the United States. But schooling, shopping, and sporting events went on as normal, and the pandemic has largely faded from public memory.
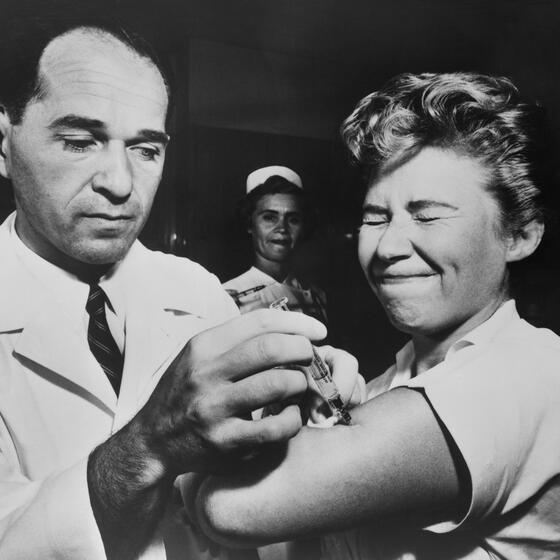
A nurse at Montefiore Hospital in New York City receives a flu vaccination in 1957. Photo: Everett Collection Historical/Alamy Stock Photo.
On April 17, 1957, the first news of a flu outbreak in Hong Kong reached an American audience, when a single column of news appeared in the New York Times on the international page. Amidst dispatches from Turkey, the UK, Greece, and Sweden, and ads for men’s tropical worsted suits and women’s silk blouses, was the headline “Hong Kong Battling Influenza Epidemic.”
Thousands of people were lining up for treatment at clinics across the British colony, many of them “refugees from Communist China.” Mothers carried their “glassy-eyed” children on their backs. Some 250,000 people were sick—about 10% of Hong Kong’s population. Officials worried that overcrowded conditions among the city’s 700,000 refugees would lead to calamity.
Epidemiologists around the world looked at Hong Kong with a sense of dread. The outbreak had happened unnervingly fast, indicating that this flu virus was unusually infectious. And while there had been small regional outbreaks of flu since the 1918 pandemic that killed perhaps 40 million people worldwide, no single pathogen had swept the world.
From our vantage point in the midst of the COVID-19 pandemic, the response to the 1957 flu is illuminating of the critical turning points that determine how a disease spreads and how it ultimately impacts society. It forced officials to make hard decisions balancing public health and potential disruption to daily life. It was the first test of a new early warning system for global outbreaks, and the first pandemic that was battled in real time with a newly developed vaccine.
The seeds of that response were planted during World War II, when the U.S. military formed a Commission on Influenzae, recruiting leading researchers from universities and hospitals. Out of that effort came the first flu vaccine, developed by Thomas Francis and Jonas Salk (Salk famously went on to develop the polio vaccine in 1952). Soldiers got the first flu shots.
In 1948, the World Health Organization established the Worldwide Influenza Centre in London at the National Institute for Medical Research—where the flu virus was first identified, in 1933—and four years later launched the Global Influenza Surveillance and Response System (GISRS), a network of 26 laboratories around the world tasked with monitoring flu evolution. And just a year before the outbreak, in 1956, the Influenza Branch of the CDC, which was only about a decade old, became a WHO Collaborating Centre for Surveillance, Epidemiology & Control of Influenza.
These systems weren’t really challenged until the flu pandemic of 1957. Experts saw the pandemic coming, and attempted to mobilize in response. But while the skeletal framework for coordinated action may have been in place, it lacked connective tissue. Samples sent from Hong Kong to the WHO in London, for example, weren’t immediately analyzed, frustrating the researchers who’d sent them.
The 1957 pandemic has largely faded from public memory. One reason may be that while many died, its mortality rate was low. It’s classified as a Category 2 pandemic—one step more severe than the seasonal flu and swine flu. (The 1918 pandemic is a Category 5. Based on its mortality rate so far, COVID-19 would be a Category 3 or 4.)
Another reason that the pandemic is forgotten may be that it struck a society more accustomed to contagious disease than we are; antibiotics and vaccines were only beginning to become more widely available as tools of public health. Moreover, even as millions became ill and thousands died, travel, school, shopping and sporting events mostly went on as normal.
Sick Sailors
In spring 1957, as the novel H2N2 virus spread through eastern Asia, American sailors in the Pacific began to get sick. The virus spread through the close quarters of ships and then military bases in Japan and Korea. Doctors had sailors gargle with a throat-wash and took samples of their blood, some of which they bottled and sent to the U.S. One of those who requested viral samples was Maurice Hilleman, the chief of respiratory diseases at the Walter Reed Army Institute of Research in Washington, D.C. Hilleman would go on to invent more than 40 vaccines over the course of his career.
While researchers were relieved to realize that they weren’t facing the same strain as the one that caused the 1918 pandemic, they were also alarmed that they had a novel strain on their hands.
Hilleman ignored federal regulations and called six vaccine manufacturers directly, advising them, “Don’t kill your roosters.” Vaccines were produced in fertilized eggs; with millions of doses to be developed, they were going to need a lot of eggs. He shipped viral samples to all six so they could get started. They promised to provide 60 million doses by February 1, 1958.
He also issued a press release from Walter Reed, warning that a flu pandemic would hit in the fall just as the new school year started.
But the flu didn’t wait for fall. By June, it had spread to 20 countries, including the U.S., where it landed on military bases first. An aircraft vessel parked at a port in southern California saw 157 crew admitted to sick bay in just two weeks. And at a naval base in San Diego, 70% of the recruits got sick. Soon there were 10,000 cases on West Coast bases alone. Across the country, at a port in Rhode Island, the flu swept through the quarters of seven destroyers.
Summer Superspreaders
In early June, hundreds of teenage girls attended a Girls State government event at the campus of the University of California, Davis. Soon enough, more than 200 of them began to shiver and burn in their dorm rooms.
“The girls feel rough for about a day as their temperatures go up to 103 and 104 but after that they snap right out of it,” the Girls State program director told a local paper. The young attendees were fine—but a 57-year-old advisor died.
One of the girls didn’t show any flu symptoms until she was on a train to Iowa with about a hundred other Californians. They were headed to an international church conference at a college in Ames with about 1,700 participants. The group was split up and housed all over campus, and soon other conference attendees fell ill. So many people were infected that the organizers cancelled the conference and sent everyone home—where they subsequently passed on the virus to others.
By mid-July, the virus’s spread in the U.S. was pretty well known by both the public and by health authorities. The CDC had created an Influenza Surveillance Unit in response, and were receiving weekly health reports from counties across the country. It also conducted a weekly national health phone survey of 2,000 persons in 700 households. Cases of people who’d spent at least a day in bed with an upper respiratory infection were flagged and sent to the CDC. Both methods documented that a pandemic was indeed underway.
Dozens of kids from California fell ill on a train to the Boy Scouts Jamboree, but weren’t turned back. Multiple clusters of cases would eventually be traced to the event.
And yet in mid July, nearly a thousand kids from California packed onto a weeklong cross-country train to Valley Forge, Pennsylvania. They were headed to the fourth annual Boy Scouts Jamboree, where 52,580 kids from 43 countries were going to bunk for a week in hundreds of tents sprawled across the Revolutionary War battlefield. Vice President Richard Nixon would greet them when they arrived, and musician Jimmy Dean—better known today for his breakfast sausages—would entertain them with his band, the Harmonica Rascals.
On the train, dozens of scouts came down with body aches, sore throats, fevers, and fatigue. Troop leaders alerted the event organizers. But instead of turning the kids back, the organizers decided to let them stay, segregating the boys in an isolated area of the park. The CDC and Pennsylvania public health officials also set up an infirmary tent for suspected flu cases.
Amazingly, there wasn’t a massive outbreak at the jamboree, but enough boys got infected that they became disease vectors when they returned to their hometowns. Multiple clusters of cases would eventually be traced back to the event, including a flu outbreak resulting from the 18 scouts who brought the virus back to Jackson, Mississippi.
Similar scenes repeated throughout the summer. One outbreak in northeast Louisiana came as schools opened in July to make up for lost classroom time in the spring, when the students harvested strawberries. Cases exploded by early August, forcing 10 schools to shut down. Nevertheless, the disease spread across Louisiana and into Mississippi.
And yet the 1957 outbreak hadn’t proved to be particularly fatal. “Most of the deaths have occurred among persons already weakened by chronic disease, old age, or hunger,” the United Press reported in late June. “The great majority of patients recover after three or four days of fever and malaise.”
“The probability of another 1918 is slight,” Carl Bauer, an influenza expert with the U.S. Public Health Service, told the UP, “but we cannot assume it is an impossibility.”
A Voluntary Allocation Plan
Even as cases ebbed in mid August, public health officials worried whether the big hit would come in September, as Hilleman had predicted, or early winter, as was typical. Anticipating the former scenario, the CDC had done intensive contract tracing in Louisiana to understand how the pandemic might play out as kids returned to school.
The surgeon general, Leroy Burney, directed that vaccine doses should be allotted to states based on population size. Soon after, public health experts from the USPHS came together in Washington, D.C., to figure out how to get the vaccine out.
They developed a “voluntary allocation” plan with vaccine manufacturers that would distribute the shots through the free market. There would be no central federal management. In theory, it was to be an equitable distribution. But as historian George Dehner writes in Influenza: A Century of Science and Public Health Response, pharmaceutical companies had already taken vaccine preorders from corporate clients such as Ford and AT&T. One pharma executive said the companies “would need to be considered in any allocation plan.”
The military had claimed the first 2.6 million doses; sailors and soldiers began to receive inoculations in August. Vulnerable populations, healthcare workers, and essential transportation, communications, and utility employees were next on the list; they needed 12 million doses. Officials launched a promotional campaign to encourage all Americans to get the vaccine once it became more widely available.
Sidelining Football Season
When schools opened in early September, flu cases exploded across the country. Schools were often the source. Kids were more susceptible than adults to H2N2; unlike COVID, the virus was less likely to infect people over age 60. Student absentee rates ranged from 30 to 60% in many communities. In New York City, tens of thousands of kids were out sick at once. But schools remained open. A health commissioner in Nassau County, New York, explained the rationale: “Children would get sick just as easily out of school.” Adults missed work at a much lower rate, but some stayed home. In hard-hit New York City, the subway system lost $1 million in revenue as sick riders skipped the commute.
Large corporations secured many of the early doses of the vaccine. By the time it was widely available, infection rates were dropping and as much as half of the vaccine was returned unused.
By late September, few vaccine doses were available compared to the size of the outbreak. The American Medical Association charged that doses were going to corporate executives rather than doctors’ patients. There were reports that football players for the San Francisco 49ers got shots but cops and firefighters didn’t.
According to Dehner, a pharma sales manager summed up the problem this way: “You got 25 people wanting apples and you only got one apple. So who gets the apple? The guy who has his hand out first.”
Public health officials monitored the outbreak but believed that “efforts to contain it were futile,” scholars at the Center for Biosecurity of the University of Pittsburgh Medical Center wrote in a 2009 paper. Rather than quarantining the infected, cancelling large events, or limiting travel, they stressed keeping the sick at home. Sick people inundated clinics, doctors’ offices and emergency rooms, but few of them needed to be hospitalized.
So normal life continued—and people got ill. By October, more than half of the counties in the U.S. had an outbreak. College football games across the country—Western Michigan vs. Colorado State, Lehigh vs. Rutgers, Navy vs. Yale, and many others—were cancelled because too many players were sick.
The cancellations coincided with the pandemic’s peak. That’s also when vaccines started to become more broadly available. But they were less than 60% effective, and they took two weeks to have a protective effect. Moreover, skeptics claimed the vaccine was worse than the disease, and some critics said the government’s vaccine promotion was a scheme to increase sales, Dehner writes.
In November, infection rates began to drop all over the country. By then, 53 million vaccine doses had been released, but the demand was low. Vaccine manufacturers sold some of it overseas, but as much as half of it was eventually returned to them, unused, according to Hillman.
At sea, it was a different story. The Pacific ships that had been struck down in the summer suffered another round of infection in November, even though their crews had been vaccinated. Sailors on two naval vessels became ill after visiting ports in Japan, which was having a major outbreak. Two more ships were stricken after visiting ports in the Philippines.
Back in the U.S., the worst of the pandemic was over. But Christmas spending was muted. A nationwide poll found that nearly half of people said they had less money because of the pandemic.
Mysterious Deaths in Winter ’58
Infection rates remained low throughout the winter of 1958, and yet death rates increased, puzzling public health officials. The CDC’s chief epidemiologist suspected it was the result of small, sporadic outbreaks that flew under the radar.
By spring, the pandemic was largely over. It’s not quite accurate to say that life returned to normal in 1958, because life had remained mostly normal. The death rate had been low, many of the cases had been mild, and there had been virtually no restrictions on daily life.
As a Pomona county health officer put it in February 1958, “The approach of the influenza pandemic across the Pacific was so well heralded that the first wave of the disorder was something of an anticlimax for many people—especially for those who missed getting it.”
And yet, H2N2 caused about 1.1 million deaths around the world in 1957–58. As many as 116,000 of them occurred in the U.S. In 1958, Met Life statisticians calculated that it had lowered the average life expectancy in the U.S. by 3.6 months, from an all-time high of 70.2 to 69.9.
Though the vaccine came too late to have much of an impact on the 1957 pandemic, its relatively fast development set a new bar—one that would be surpassed in 1968, which saw another flu pandemic that began in Hong Kong. That vaccine was ready in 66 days.