Did Congress Just Fix Surprise Medical Billing?
The omnibus spending and COVID relief bill signed by President Donald Trump on December 27 includes a measure to prevent patients from being billed by out-of-network doctors after treatment in an in-network hospital—a practice that frequently landed patients with huge, unexpected debts. We asked Prof. Fiona Scott Morton, whose research helped bring the practice to light, what the new law will mean for patients and healthcare costs.
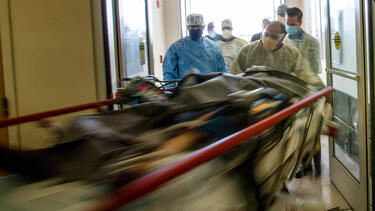
An emergency room in Moreno Valley, California, in May 2020. Photo: Gina Ferazzi/Los Angeles Times via Getty Images.
What has your research shown about the scale of surprise billing in the U.S.?
Professor Zack Cooper and I showed that about 20% of ED visits come with a surprise physician bill but that those cases were concentrated at a small proportion of hospitals. Those “problem” hospitals were more likely to be smaller, for profit hospitals that had contracted with an ED physician staffing company such as TeamHealth or Emcare. These companies specialize in removing their doctors from insurers’ networks and then demanding high prices. In the case of TeamHealth, they sometimes returned to in-network status in exchange for a somewhat higher price. But Emcare physicians tend to stay out of insurers’ networks entirely and bill at three times the Medicare rate. The insurers would refuse to pay, leaving patients to be pursued by physicians for these very high charges. We also found out that both TeamHealth and Emcare were owned by private equity companies, presumably because they had figured out how lucrative surprise billing could be.
“The cost of arbitration will stop bad actors from setting up in business—the way they do now—with a strategy of staying out of network and demanding very high prices.”
States are limited in what they can regulate. New York, which we study, moved early to prohibit surprise billing and require arbitration. However, that law technically could only apply to fully insured plans, which are less than half of all bills. So a state-level solution was not ideal.
Do you think the solution added to the stimulus bill will solve the problem?
Yes, it will. First, it will hold the patient harmless, which means she will pay whatever she would pay for an in-network charge. That’s key. Then the insurer and doctor get to fight over who pays the balance in arbitration. The arbitrator is instructed to look at local negotiated rates rather than “charges,” an arbitrary list price chosen by the physician, or Medicare rates which are chosen by the government.
Arbitration has costs, of course, but the process is likely to generate something fair. And the cost of arbitration will stop bad actors from setting up in business—the way they do now—with a strategy of staying out of network and demanding very high prices. Those very high prices will not make it through arbitration, so that business model will stop being attractive.
The law will lower healthcare costs because these high payments will disappear, but it will also reduce healthcare costs because the out-of-network physicians were using many more hospital services and tests. This drove up revenue of the hospitals that allowed surprise billing and might be why they did not work to get rid of it.
Why did it take so long to get a federal law prohibiting surprise billing?
It is interesting that a practice we have known about for a number of years was allowed to thrive for so long. Neither Republicans nor Democrats liked it, nor did patients, advocacy groups, and many doctors and hospitals. But reform was stymied for a number of years due to the power of a congressman from western Massachusetts, Richard Neal, who chairs the House Ways and Means committee. He received donations to his campaign from those who profited from surprise billing —the previously mentioned private equity firms and hospitals—and blocked reform until Speaker Pelosi finally intervened. This phenomenon illustrates why our political system makes it difficult to lower U.S. healthcare costs. Those expenditures are always someone’s income, and that business lobbies to stop reforms that would save patients and taxpayers money. Lobbying works!